Trauma Impacts Clients
What Is Trauma-Informed Care?
It is "...care that understands and considers the pervasive nature of trauma and promotes environments of healing and recovery rather than practices and services that may inadvertently re-traumatize."
The Institute of Trauma and Trauma-Informed Care states that there are five guiding principles in Trauma-Informed Care. These are safety, choice, collaboration, trustworthiness, and empowerment.
Creating safety is both a physical and emotional experience. Many healthcare professionals are unaware of how to create a safe space for clients who are emotionally vulnerable. Nikki Estep, a diabetes care and education specialist, explains helping the client feel heard is essential. Attending an education session typically is about the professional transferring knowledge to the client. This can make the client feels talked ‘at’ and if they aren’t monitoring blood sugar or moderating carbohydrate intake the experience may be perceived as a ‘talking to’ instead of engaging in a collaborative session.
Shifting how the educational experience is described is a helpful step. The client is no longer told’ what to do but is provided with an opportunity to form and share how they wish to manage their diabetes.
Choice, trustworthiness, and empowerment continue the foundation of Trauma-Informed Care. These next three qualities of Trauma-Informed Care are free of coercion because they focus on the client’s ability to make the best choice for them, and they decrease emphasis on achieving a specific outcome. This shift is hard for most healthcare providers who by training are number-focused. Diabetes is a great example of a number-focused chronic illness. The numbers include evaluating multiple times a day carbohydrates at meals, daily blood glucose monitoring, quarterly A1C, and HDL and Triglyceride goals. Many providers also insist on monitoring weight even when the client does not have kidney disease or congestive heart failure. This shift away from the client to reemphasize outcomes is the consequence of brief medical visits that lack sufficient time for the healthcare provider to reestablish a humanistic connection.
Read More
Learn more with our free ebook
Download our free ebook so you can learn more about Trauma-Informed Care and Diabetes.
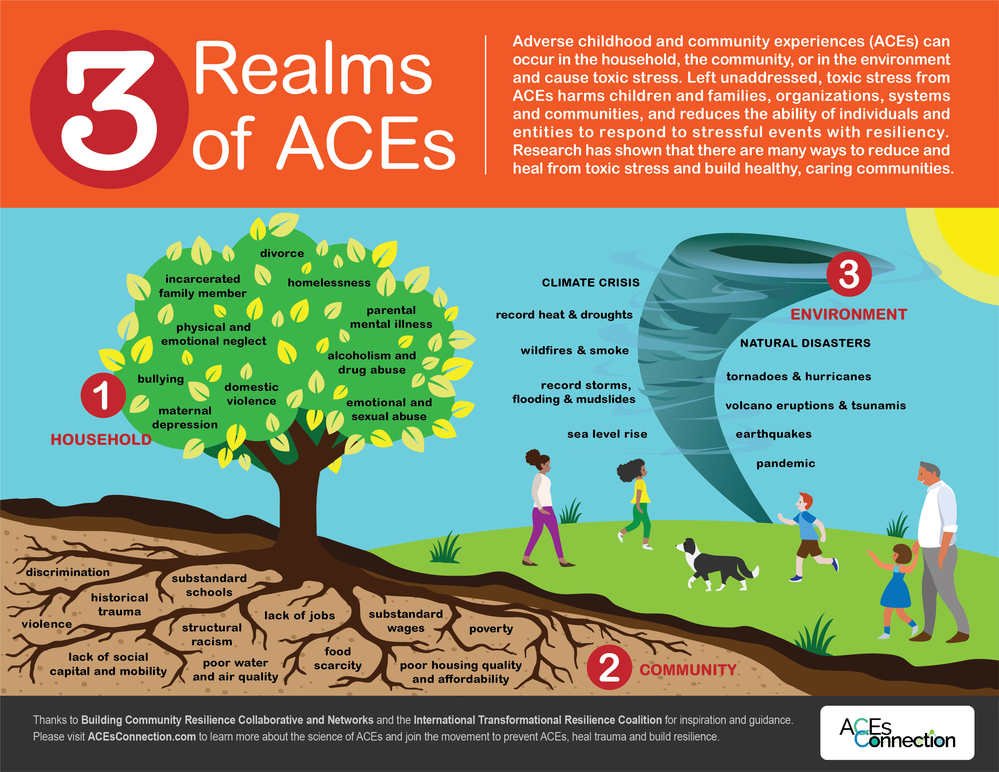
Many Types of Trauma
There are many things that can be considered Trauma. The Adverse Childhood Experience, ACE research looked at 10 things. Since 1985 the research regarding adversity, trauma, and resilience has increased. The image to the left shows three categories of trauma. These are Households, Communities, and Environment.

